Diuretic DefinitionA diuretic is any drug that promotes diuresis or increased urine production. This includes limited diuresis. A diuretic pill is colloquially known as a water tablet. Diuretics are classified into several types. All diuretics increase water excretion from the body via the kidneys. An antidiuretic, on the other hand, such as vasopressin (antidiuretic chemical), is a specialist or drug that decreases the outflow of water in urine. 
Medical UsesDiuretics are used in medicine to treat cardiovascular disease, liver cirrhosis, hypertension, the flu, water toxicity, and some kidney diseases. A few diuretics, for example, acetazolamide, serve to make the pee more basic and are beneficial in increasing the discharge of chemicals, for example, ibuprofen, in cases of excess or injury. Diuretics are frequently used by those with a food problem, notably those with bulimia nervosa, who are desperate to lose weight. Some diuretics' antihypertensive properties (particularly thiazides and circle diuretics) are diuretic-free. The drop in pulse isn't caused by decreased blood volume due to increased urine production but rather occurs through alternative routes and at lower parts than those thought to supply diuresis. Indapamide was explicitly planned considering this, and it offers a more extensive remedial window for hypertension (without enunciated diuresis) than most different diuretics. Types of Diuretics1. Loop Diuretics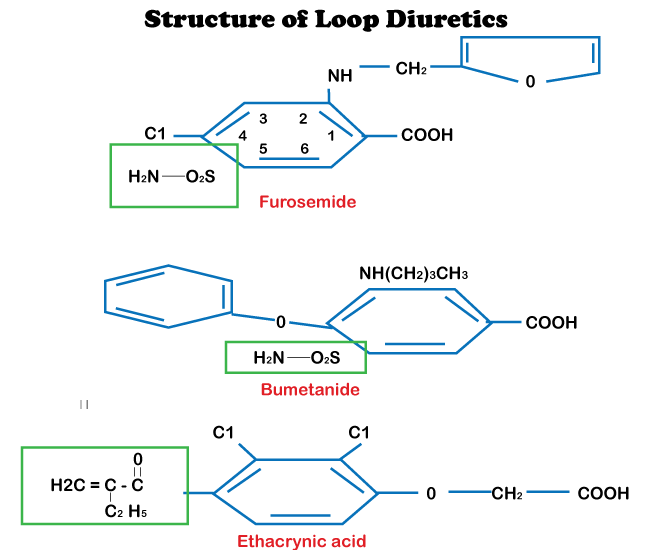
High-roof diuretics may produce significant diuresis - up to 20% of the sifting heap of NaCl (salt) and water. Circle diuretics have this ability and are hence commonly inseparable from high-roof diuretics. Circle diuretics, such as furosemide, limit the body's ability to reabsorb sodium at the rising circle in the nephron, causing a release of water in the urine. In contrast, water normally accompanies sodium back into the extracellular fluids. Other examples of high-roof circle diuretics are ethacrynic corrosive and torasemide. 2. Thiazides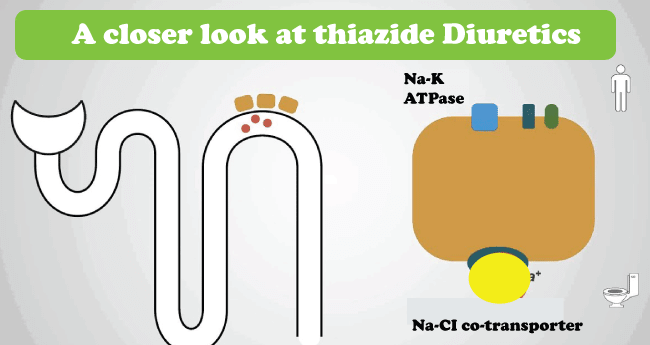
Thiazide-type diuretics, such as hydrochlorothiazide, act on the distal convoluted tubule and inhibit the sodium-chloride symporter, causing water to accumulate in the urine since water normally goes with entering solutes. The increased body water loss due to a coordinated interaction with sodium setback from the tangled tubule induces prolonged urine. Thiazides are a transient antagonist of hypertensive action due to their ability to diminish preload and hence lessen circulatory strain. The delayed impact, however, is due to an unknown vasodilator action that reduces circulatory strain by reducing the obstruction. 3. Carbonic Anhydrase Inhibitors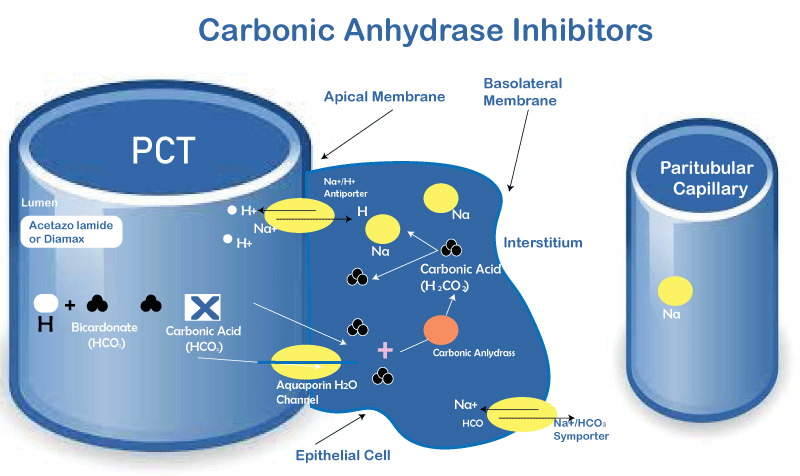
Carbonic anhydrase inhibitors block the chemical carbonic anhydrase in the proximal tangled tubule. This has a few consequences, including increased bicarbonate collection in the urine and decreased salt retention. 4. Potassium-Sparing Diuretics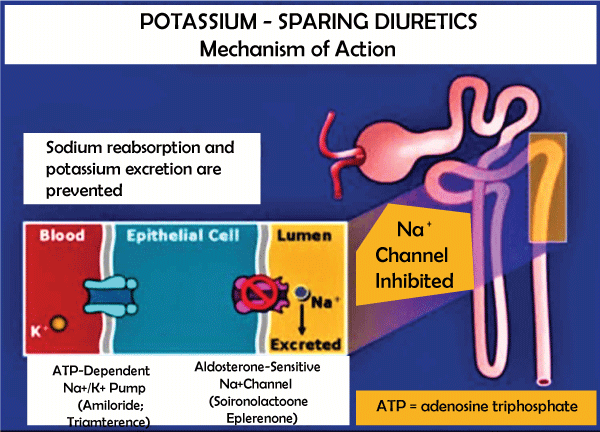
These diuretics don't accelerate the arrival of potassium into the pee; accordingly, potassium is held and not lost as much as with different diuretics. The word "potassium-saving" refers to an effect rather than an instrument or location; in any event, the term frequently refers to two specified classifications that influence comparable areas:
5. Osmotic Diuretics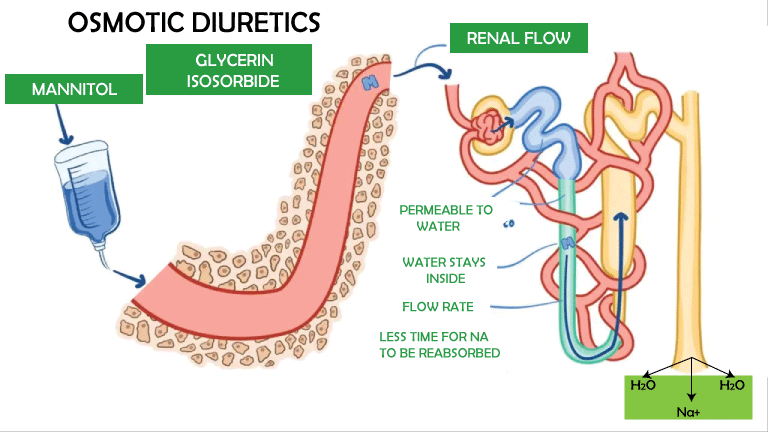
Osmotic diuretics are medications that promote osmolarity while penetrating only partially into cylindrical epithelial cells. They primarily raise extracellular liquid and plasma volume, boosting blood flow to the kidney, namely the peritubular arteries. This reduces medullary osmolality, preventing urine fixation in Henle's circle (which typically utilizes the high osmotic and solute slope to move solutes and water). Moreover, the porousness of the restricted cylindrical epithelial cell enhances osmolality and, as a result, water retention in the filtrate. It was recently discovered that the primary feature of osmotic diuretics like mannitol is that they are isolated in the glomerulus but cannot be reabsorbed. As a result of their presence, the osmolarity of the filtrate rises, and water is retained in the urine to maintain osmotic equilibrium. Glucose, as opposed to mannitol, is typically detected in the blood. Nevertheless, in some situations, such as diabetes mellitus, the blood glucose concentration (hyperglycemia) surpasses the kidney's maximal reabsorption capacity. When this occurs, glucose stays in the filtrate, causing osmotic water retention in the urine. Glucosuria is brought about by the deficiency of hypotonic water and Na+, bringing about a hypertonic state with volume consumption signs such as dry mucosa, hypotension, tachycardia, and diminished skin turgor. Certain medicines, particularly stimulants, can cause a rise in blood glucose and hence an increase in urine. Precautions for DiureticsVisiting a doctor regularly when taking a diuretic is important. The doctor will examine the drug to ensure it works properly and look for any negative side effects. When people first start taking diuretics, they may feel abnormally exhausted. This impact is normally less recognizable in the long haul as the body acclimates to the medication. Since diuretics increment pee yield, individuals who take this medication might have to pee more regularly, particularly around evening time. Experts in medical services can help individuals organize their doses so that they do not disturb their rest or usual workouts. Doctors may recommend adding potassium-rich food sources or beverages, such as citrus goods, from the soil to the eating pattern of patients on diuretics that deplete potassium from the body. On the other side, they may recommend taking a potassium supplement or another prescription that prevents the body from losing a lot of potassium. If the doctor recommends any of these steps, pay close attention to the headers. Avoid making any additional dietary modifications without first seeing your doctor. People on potassium-saving diuretics should avoid adding potassium to their weight-loss efforts since an excess of potassium may be harmful. When people who take diuretics feel unwell, they may lose a lot of water or potassium, particularly if they have severe retching and loose stools. If they feel ill, they should consult with their doctors. When some people stand up after sitting or resting, they feel disoriented, queasy, or faint. Consuming alcohol, working out, representing for lengths, or being outside in hot temperatures may increase the problem. To alleviate the problem, get up gradually and, if possible, grasp something for assistance. Avoid excessive alcohol consumption and exercise caution in hot weather or while practising or representing for an extended period. Before undergoing cautious or dental systems, clinical trials, or crisis therapy, everyone using a diuretic should notify the medical services expert in control. Several diuretics make the skin more sensitive to sunlight. Moreover, even brief exposure to the sun can cause acute sunburn, shivering, rash, redness, or other changes in complexion. While using this drug, avoid being in direct sunlight, especially between 10 a.m. and early afternoon. Moreover, at 3 p.m., wear a cap and securely woven dress that covers the arms and legs; use sunscreen with a skin insurance factor (SPF) of no less than 15; shield the lips with a sun block lipstick; and don't use tanning beds, tanning corners, or sunlamps. Special ConditionsPeople with particular illnesses or taking certain medicines may experience complications if they take diuretics. Before using these drugs, notify your doctor if you have any of the following conditions:
Those with bronchial asthma are more likely to develop hypersensitivity to particular diuretics. Anyone with these clinical concerns should inform their doctors about their situation before using diuretics. Those who have difficulties urinating or have excessive potassium levels in their blood will also be unable to use diuretics and should see a doctor before using them. Particular Prescriptions are used. Using diuretics alongside some other drugs may affect how the treatments operate or increase the possibility of side effects.
Next TopicTime Period Definition
|
 For Videos Join Our Youtube Channel: Join Now
For Videos Join Our Youtube Channel: Join Now
Feedback
- Send your Feedback to [email protected]
Help Others, Please Share










