What is the Full Form of SIR(i) SIR: Society of Interventional RadiologySIR stands for Society of Interventional Radiology. It is a national medical, scientific, and allied health organization in the United States devoted to promoting public health via the use of minimally invasive, image-guided therapeutic therapies for disease management. 
The Society of Cardiovascular Radiography was started in 1973 by an active group of radiologists who wished to advance interventional elements of radiology. In 1983, it was renamed the Society of Cardiovascular and Interventional Radiology. The name was changed to the Society of Interventional Radiology in April 2002 to reflect the growing relevance of interventional radiology, which is no longer restricted to the cardiovascular system. As of March 2017, the society had around 7000 members: practising physicians, trainees, scientists, and clinical associates such as physician assistants, nurse practitioners, radiologic technicians, and paramedics. The first female president was Katharine L. Krol. The official journal of SIR is the Journal of Vascular and Interventional Radiology. (ii) SIR: Silent Information RegulatorSIR also stands for Silent Information Regulator. These are proteins involved in the regulation of gene expression. They organize heterochromatin at telomeres, rDNA, and quiet loci, including concealed mating type loci in yeast. The SIR gene family encodes catalytic and non-catalytic proteins involved in histone tail deacetylation and subsequent chromatin condensation around a SIR protein scaffold. Some members of the Silent Information Regulator family are found in both yeast and humans. 
Anita Hopper and Benjamin Hall produced one of the first yeast screens to find SIR genes, using mutagenesis to look for alleles that allowed sporulation in a typically sporulation-deficient heterothallic Strain (ho/ho MAT/MAT). Their screen uncovered a mutation in a new gene unrelated to HO that allowed the / diploid to sporulate as if it were a /a diploid, demonstrating that the mutation affected mating type through an HO-independent mechanism. It was later determined that Hopper and Hall's CMT mutation did not result in a MAT gene mating type conversion. Instead, it enabled the expression of cryptic mating-type genes that were previously silenced in wild-type yeast. Haber thanked Amar Klar's assistance in his study elucidating the mechanism of the CMT mutation. At the Cold Spring Harbor Laboratory yeast genetics symposium, the latter presented his MAR mutant strains with features similar to the CMT mutants, causing Haber to consider if the CMT mutants work by suppressing silent information. Two more groups published screens for genes involved in the control of silent mating type cassette tapes the same year. Haber discovered that de-repressing hidden mating type loci restored sporulation in the CMT mutant. Amar Klar, Seymour Fogel, and Kathy Macleod discovered a mutation in an a/a diploid that resulted in haploids with an apparent diploid phenotype as measured by pairable characteristics. The mutation, the researchers reasoned, de-repressed the previously discovered silent mating type loci HMa and HM, allowing an a/a diploid to sporulate and haploid segregants receiving the mutant allele to operate as a/diploids despite being haploid. The authors termed the mutation MAR because of its claimed significance in mating type regulation, were able to map it to chromosome IV, and concluded that it was positioned 27.3 cm from a regularly used trp1 marker. Several months later, Jasper Rine and Ira Herskowitz released a new screen for genes that modified yeast's ability to pair, finally identifying the SIR gene family, which is still utilized today. Unlike the Klar et al. screen, which discovered a mutant based on its inability to pair, Rine and Herskowitz employed a more targeted strategy to identify components involved in mating type suppression. Rine and Herskowitz reasoned that by de-repressing the silent copy of MAT, a haploid yeast cell with a recessive mutation in mat1 might be integrated. Rine and Herskowitz started with a haploid ho mat1 strain. They looked for mutagenesis mutants and discovered five that restored the MAT phenotype in mat cells but were unrelated to the MAT locus and did not result in a gene conversion between the HM locus and mat. They reasoned that the cryptic mating-type genes were significantly suppressed in these mutants. All of the mutants identified by the first Hopper & Hall screen, as well as the later Rine & Herskowitz and Klar et al. screens, were subsequently characterized and mapped. According to the screen that found the mutations, the genes currently known as SIR1-4 were previously known as MAR, CMT, or STE. (iii) SIR: Selective Internal RadiationSIR also stands for Selective internal radiation, commonly known as transarterial radioembolization (TARE). It is a type of radiation treatment used to treat cancer in interventional radiology. It is typically reserved for patients with surgically unresectable malignancies, notably hepatocellular carcinoma or liver metastases. The therapy involves injecting microscopic radioactive microspheres into the arteries that nourish the tumour, where the spheres lodge in the tumour's tiny capillaries. This technique is also known as radioembolization since it combines radiation and embolization. Chemoembolization is the chemotherapeutic counterpart, and the most frequent version is transcatheter arterial chemoembolization. 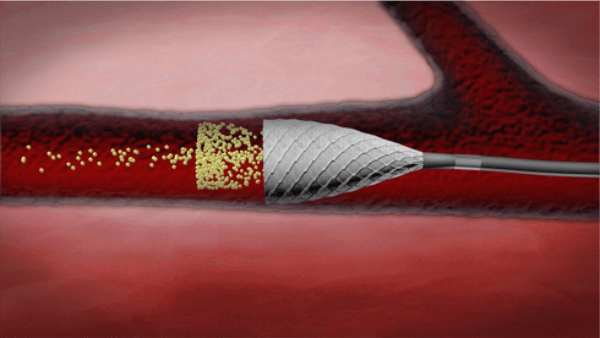
Radiation treatment destroys cancer cells, but it also sometimes damages normal cells. Currently, therapeutic amounts of radiation may be precisely targeted to tumours using linear accelerators in radiation oncology. However, while irradiating using external beam irradiation, the beam must always pass through healthy tissue. Radiation can cause damage to normal liver tissue. The liver parenchyma's radiation sensitivity restricts the radiation dosage that may be supplied using external beam radiotherapy. On the other hand, SIR entails physically injecting radioactive microspheres into a location, leading to local and targeted radioactive dose deposition. As a result, it is well-suited for the treatment of liver tumours. SIR is classified as a locoregional treatment (LT) due to the local deposit. The liver receives blood from two sources: the portal vein and the hepatic artery. The portal vein primarily perfuses healthy liver tissue. The hepatic artery, on the other hand, is responsible for supplying blood to the vast majority of liver tumours. As a result, locoregional treatments such as transarterial chemoembolization or radioembolization can be delivered selectively in the arteries supplying the tumours and preferentially lead to particle deposition in the tumour while sparing good liver tissue from detrimental side effects. Furthermore, malignancies are frequently hypervascular; tumour blood supplies are enhanced in comparison to normal tissue, resulting in preferential particle deposition in tumours. Selective Internal Radiation therapy can be done in a variety of ways, including whole-liver therapy and lobar or segmental methods. Full hepatic Selective Internal Radiation is a therapy that targets the entire liver in one session and can be utilized when the illness has progressed throughout the liver. When treating the entire liver in two distinct treatments, one lobe at a time, it might be a suitable therapeutic choice when only a single lobe is implicated. The segmental method, also known as radiation segmentectomy, is a procedure that delivers a high dosage of radiation to only one or two Couinaud liver segments. The increased amount results in the eradication of the tumour. While at the same time, the damage to healthy liver tissue is limited to the targeted areas. This method causes effective necrosis of the targeted parts. Segmentectomy may be performed when the tumour (s) are in one or two pieces.
Next TopicFull Form
|
 For Videos Join Our Youtube Channel: Join Now
For Videos Join Our Youtube Channel: Join Now
Feedback
- Send your Feedback to [email protected]
Help Others, Please Share










