Black Fungus (Mucormycosis)
From last 2019, the world has been going through a pandemic. A virus named corona has captured the whole world, and still, we all are fighting with it. Within this period, another disease attack on humans infected the human eye and resulted in death. This disease is named Mucormycosis (black fungus). After COVID-1, millions of people constantly fought and compromised over low immune systems. In these fatal conditions, a brutal fungus - mucormycosis took the advantage. This disease is caused by fungi that attack the person having low immunity via inhalation of spores from the surrounding area. It's not a contagious fungal infection, but it infects the nose, sinuses, brain, and eye. These fungal spores can be transmitted in a hospital or during drug use. Mucormycosis is a dangerous infection that is a pathogen that colonises blood vessels resulting in blood clots (thrombosis) and death of tissues (tissue necrosis). A group of molds called micromycetes causes this, and humans inhale these molds spores come in contact with things like rotting procedures or bread, soil, or compost piles. 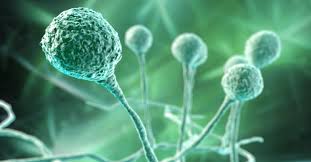
History
Note:- First case of mucormycosis was reported in the Chikkamagaluru district. More than 557 cases were reported in urban Bengaluru. Other cases have been reported in Karnataka, around 1370 cases of mucormycosis in which more than 51 people lost their lives.Mucormycosis symptomsIn the human body, mucormycosis symptoms arise at a different part of the body where the fungus grows. Symptoms are:-
This fungal infection spreads all over the body through blood circulation called as disseminated mucormycosis. It affects the spleen, heart, and skin (the infected part of the skin turns black and feels warm and painful). In some severe cases, it can affect the patient's mental state and arise the condition of coma or even be deadly. 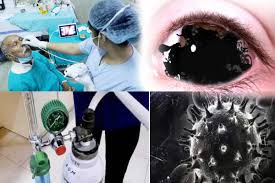
Note:- Multiple fungi can cause mucormycosis called mucormycetes belongs to mucorals. A common type of mucormycetes is- Rhizopus species and Mucor species. Some other examples are - Syncephalastrum species, Apophysomyces, Lichtheimia (formerly Absidia), Saksenaea, Cunninghamella bertholletiae, and Rhizomucor. Rather fungi are not infectious or harmful for most people but not for everyone. Fungal infection is risky for:-Mucormycosis can infect any age group of people that come in contact with fungus in their everyday lives. It commonly attacks the person having weak immune system or already on medication due to health conditions like:-
PreventionVarious preventive measures should be taken for black fungus.
There are some do's and don't people should follow:- Results of mucormycosisBlack fungus infection left deadly results without treatment on time because this infection is rare, and 54% of people with mucormycosis die. The death rate depends on the infected part of the body (which part is affected more). Mucormycosis complications include:-
Diagnosis of mucormycosisPatients with a low immune system and suffered from COVID-19found to be easily attacked by mucormycosis. Initial symptoms should not be avoided; humans are advised to visit the doctor as soon as possible. Doctor follow the procedure:-
Treatment of mucormycosisAfter detection of mucormycosis disease, immediate treatment should be started by taking prescribed antifungal medications that stop the development of fungus, control it and destroy it from the body. Some prescribed medicines are:-
These medicines should be taken at the correct time with all the precautions (dosage, timing). In case of high infection, doctors can increase the dose of pills that can take several weeks to control infection. Intravenous antifungal curing procedures can take 4-6 weeks. In most complicated, doctors can recommend surgery (removing dead tissue or infected tissue, removing the body part). We can't figure out the surgery because it's crucial to treat this deadly (life-threatening) infection. If treatment results in stomach pain, trouble breathing, or heartburn, the doctor can change the treatment plan.
Next TopicCattle farming
|
 For Videos Join Our Youtube Channel: Join Now
For Videos Join Our Youtube Channel: Join Now
Feedback
- Send your Feedback to [email protected]
Help Others, Please Share









