Blood Clots in the BrainWhat are Blood Clots?A blood clot, often referred to as a thrombus, is a gelatinous mass created when blood components collect together as a result of an injury or other irregularities in the circulatory system. It is essential for limiting excessive bleeding and accelerating wound healing. Blood clots can, however, become problematic and pose serious health hazards in certain circumstances. Understanding the components of blood is crucial. Red blood cells, white blood cells, platelets, and plasma make up blood. Small, disk-shaped cells called platelets aid in the beginning of the clotting process. Platelets quickly build up at the site of injury in damaged blood arteries to provide a temporary stopper. Primary haemostasis is the term used to describe this initial clotting response. 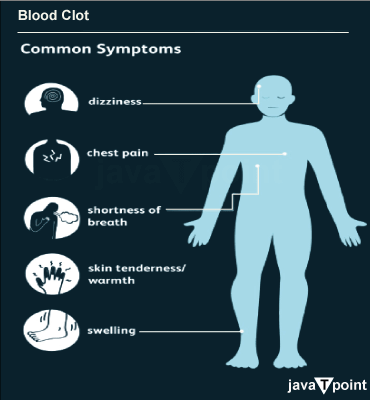
A complicated series of metabolic processes are simultaneously started in order to strengthen the platelet plug and create a stable blood clot. Secondary haemostasis is the process by which dormant proteins are changed into active enzymes through a series of protein interactions. A fibrin mesh that reinforces the platelet plug and draws in more platelets and red blood cells to create a stable clot is the result. When they form in response to wounds, blood clots are advantageous because they aid in stopping excessive bleeding and speed up tissue repair. However, issues occur when blood clots develop inadvertently within blood vessels, obstructing regular blood flow. Serious medical disorders such deep vein thrombosis (DVT), pulmonary embolism (PE), stroke, or heart attack can develop as a result of these aberrant blood clots. When a clot develops in the deep veins of the legs or pelvis, deep vein thrombosis takes place. This syndrome is frequently linked to extended periods of immobility, like those seen on lengthy flights or post-operative bed rest. A pulmonary embolism can occur if a blood clot escapes from the veins and moves through the bloodstream to the lungs. This disease necessitates quick medical attention since it could be fatal. Arterial thrombosis can occur when blood clots develop within arteries. This may lead to obstructions that prevent blood from reaching essential organs, resulting in organ malfunction or tissue damage. A blood clot in the coronary arteries, for instance, can result in a heart attack, whereas one in the cerebral arteries can result in a stroke. Blood clot risk is increased by a number of variables. These include long-term immobility, age, obesity, smoking, hormonal changes (such as those that occur during pregnancy or while taking birth control), and genetic predispositions. Additionally, thrombophilia, a genetic propensity for unnatural clotting, may exist in some people. Blood Clotting of BrainThe brain's blood clotting process is comparable to that of other bodily regions. Platelets quickly assemble at the location of a broken or aberrant blood artery in the brain to form a temporary stopper. Primary hemostasis, the first stage of clot formation, occurs at this time. In parallel, a complicated series of biochemical processes known as secondary hemostasis are started in order to strengthen the platelet plug and create a solid clot. Blood clots in the brain can form as a result of a variety of circumstances. 
The risk of blood clot formation can be increased by a number of medical disorders, including high blood pressure, diabetes, obesity, and atherosclerosis (hardening of the arteries). Additionally, immunological diseases, hormonal changes (such those that take place during pregnancy or while taking hormone replacement treatment), and genetic predispositions can also contribute. Depending on where and how big the clot is in the brain, different symptoms may be present. Seizures, a severe headache, abrupt and severe dizziness, visual problems, difficulty speaking or understanding speech, weakness or paralysis on one side of the body, and difficulty speaking or understanding speech are common indicators. If any of these symptoms appear, it is crucial to get medical aid right once because timely care can lessen the possibility of brain damage. The study of the patient's medical history, a physical examination, and imaging tests are frequently combined to make the diagnosis of blood clotting in the brain. Detailed images of the brain and blood vessels can be obtained using imaging techniques like computed tomography (CT) scans, magnetic resonance imaging (MRI), or cerebral angiography, which can be used to detect the existence and location of blood clots. Blood clotting in the brain is normally treated using a multifaceted strategy. The use of thrombolytic treatments to break the clot, anticoagulants to stop additional clot formation, and antiplatelet drugs to stop platelets from adhering to one another may all be part of immediate medical intervention. To remove or bypass the clot, surgical intervention may be necessary in some circumstances. The severity of the injury and the patient's general condition will determine recovery and long-term management following a blood clot in the brain. Physical therapy, speech therapy, and occupational therapy are examples of rehabilitation therapies that can assist regain lost function and enhance quality of life. Future clotting episodes can be avoided with lifestyle changes like keeping a healthy weight, getting regular exercise, eating a balanced diet, and taking your medications as prescribed. Management of underlying medical disorders and the elimination of identified risk factors are key components of prevention measures for blood clotting in the brain. This may entail controlling cholesterol, blood sugar, and blood pressure in addition to giving up smoking and leading a healthy lifestyle. Healthcare professionals may provide blood-thinning drugs to high-risk patients to assist avoid the formation of clots. Types of Blood Clots in the BrainThe various types of blood clots that can occur in the brain, their causes, symptoms, and available treatment options. Ischemic Stroke: An ischemic stroke is the most prevalent kind of blood clot in the brain. This happens when a clot plugs or narrows an artery, which causes blood flow to a specific area of the brain to significantly decrease or stop entirely. Atherosclerosis, which is characterised by the accumulation of fat deposits termed plaques within the arteries, frequently contributes to ischemic strokes. Smoking, diabetes, high blood pressure, and leading a sedentary lifestyle are other risk factors. Aside from sudden numbness or paralysis on one side of the body, other symptoms may include trouble speaking, excruciating headaches, and eyesight issues. Transient Ischemic Attack (TIA): When a blood clot momentarily stops an artery in the brain, a transient ischemic attack, commonly referred to as a "mini-stroke," takes place. Although technically not a stroke, TIAs should still be addressed seriously because they are warning symptoms. Although TIA symptoms resemble those of an ischemic stroke, they typically go away within 24 hours. Early medical intervention is essential since TIAs can signal a more serious stroke. Hemorrhagic Stroke: Haemorrhagic strokes, as opposed to ischemic strokes, are brought on by brain haemorrhage. Damage to brain tissue results when a blood clot in a frail or burst blood artery starts bleeding. Aneurysms (weakening blood vessel walls) and arteriovenous malformations (AVMs), which are improper connections between arteries and veins, are the most frequent causes of hemorrhagic strokes. A sudden and severe headache, vomiting, convulsions, and loss of consciousness are some possible symptoms. Cerebral Venous Sinus Thrombosis: When a blood clot forms within the venous sinuses, which are in charge of removing deoxygenated blood from the brain, this condition is known as cerebral venous sinus thrombosis (CVST). Despite being very uncommon, CVST can be fatal. It might be brought on by genetic disorders, the use of oral contraceptives, hormonal imbalances, infections, or head trauma. Severe headaches, visual abnormalities, seizures, and focal neurological impairments are just a few of the symptoms that can vary greatly. Embolic Stroke: Embolic strokes take place when a blood clot, or embolus, develops in one area of the body and moves through the bloodstream before settling in a blood vessel in the brain. The heart, where blood clots from diseases like atrial fibrillation may cause them, and big arteries, where plaques can splinter off and lodge in the brain's smaller blood channels, are the two most prevalent locations for emboli. The presence of abrupt weakness or paralysis on one side of the body, bewilderment, and trouble speaking are among the symptoms, which vary depending on where and how big the blood clot is. Treatment of Blood Clots in the BrainThe use of anticoagulant drugs is one of the main treatments for blood clots in the brain. These drugs, like heparin or warfarin, function by obstructing the development of fresh clots and preventing the expansion of existing clots. To lower the risk of future complications, anticoagulant medication is typically started as soon as feasible after the identification of a blood clot in the brain. Depending on the particular situation and the underlying reason for the clot, the anticoagulant treatment's length may change. Blood clots in the brain can sometimes be treated using thrombolytic therapy, also referred to as clot-busting therapy. Intravenously administered thrombolytic drugs, such as tissue plasminogen activators (TPAs), are used to dissolve the clot and reestablish blood flow to the damaged part of the brain. This treatment is time-sensitive, and it works best when started shortly after the first sign of symptoms. However, there is a chance that using thrombolytic therapy will result in bleeding issues, therefore it is important to carefully weigh the benefits and dangers before using it. The blood clot in the brain may occasionally need to be removed or broken up mechanically. Endovascular thrombectomy is a minimally invasive technique in which the clot in the afflicted blood vessel is physically removed using catheters and other specialised equipment. This treatment can be quite efficient at restoring blood supply to the brain and is frequently carried out by interventional radiologists or neuro-interventional surgeons. The management of blood clots in the brain must also include supportive care. This may involve closely monitoring vital signs, sustaining ideal blood pressure and oxygenation levels, and addressing any related issues. Rehabilitation therapy may be required in stroke instances brought on by a blood clot in order to assist patients restore lost function and enhance their quality of life. Preventive Measures to be Taken to Avoid Blood Clotting in BrainPreventing blood clots in the brain is essential to maintain good brain health and reduce the risk of serious complications such as stroke or brain damage. Maintain a Healthy Lifestyle: Maintaining a healthy lifestyle is essential to avoiding brain blood clots. Regular exercise lowers the risk of blood clot development and helps to enhance blood circulation. At least 30 minutes a day of physical activity, such as walking, jogging, or swimming, can be useful. The risk of blood clots can be decreased overall by keeping a healthy weight, consuming a balanced diet high in fruits, vegetables, and whole grains, and abstaining from excessive alcohol use. Stay Hydrated: Maintaining healthy blood circulation and avoiding blood clots require staying well hydrated. Throughout the day, drinking enough water keeps the blood thin and keeps it from getting too viscous. It is advised to drink at least eight glasses of water every day, or more in hot weather or when participating in vigorous activities. Quit Smoking: Smoking significantly increases the chance of developing blood clots and other cardiovascular disorders. Blood arteries can become damaged by the chemicals in cigarette smoke, which can also increase the risk of blood clotting. Reducing the incidence of blood clots in the brain and enhancing general health require quitting smoking or minimising exposure to second-hand smoke. Manage Underlying Medical Conditions: Blood clots in the brain are more likely to occur when certain medical disorders are present. To reduce the risk, it's critical to effectively handle these situations. Through medication, lifestyle changes, and routine medical exams, conditions like hypertension, diabetes, excessive cholesterol levels, and atrial fibrillation should be well treated. Effective management of these illnesses depends on adhering to the prescribed treatment regimens and maintaining regular contact with medical providers. Take Breaks During Prolonged Immobility: Long-term immobility can raise the risk of blood clot formation, such as while sitting still for extended periods when travelling or working at a desk. It's crucial to constantly take breaks and walk about. Simple exercises that increase blood circulation and avoid clotting include stretching, walking, and flexing the legs and feet. Use Compression Stockings: Compression socks or stockings are form-fitting garments that exert little pressure on the legs. They aid in enhancing blood circulation in the lower limbs, lowering the danger of blood clots. For those with a high risk of blood clots or a history of clotting issues, compression stockings are especially advantageous. It is advised to consult a healthcare practitioner to choose the right compression stocking kind and fit. Medication and Treatment: People who are at a high risk of developing blood clots in the brain may occasionally need to take medication or receive treatment to do so. This may entail taking anticoagulant drugs or antiplatelet medications as directed by a medical specialist. To ensure that the therapy is both effective and safe, it is crucial to rigorously adhere to the recommended dosage and schedule and to keep all scheduled follow-up sessions.
Next TopicBlood Supply to the Brain
|
 For Videos Join Our Youtube Channel: Join Now
For Videos Join Our Youtube Channel: Join Now
Feedback
- Send your Feedback to [email protected]
Help Others, Please Share









